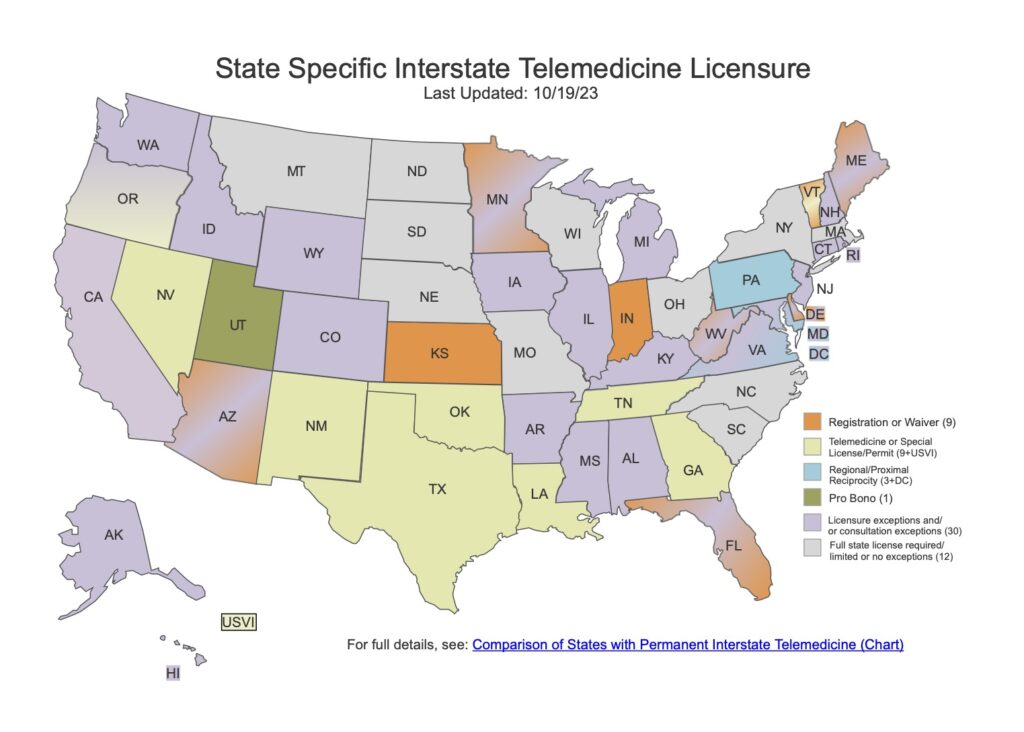
In 30 states, you can’t use telehealth with out-of-state doctors

At the height of the COVID-19 pandemic, when all 50 states and the federal government declared public health emergencies, telehealth became a lifeline for Americans. Now, to patients’ dismay, most states have rolled back telehealth access—disrupting care and putting lives at risk.
Emergency telehealth waivers
Telehealth, or telemedicine, allows patients to have virtual appointments with doctors across the country. Before the pandemic, telehealth was strictly regulated everywhere: State laws required doctors to be licensed in the state to practice medicine, even via telehealth. A New Jersey patient couldn’t have a video appointment with a renowned Boston specialist unless that specialist got licensed in New Jersey—an intensive three-month process that requires renewal and continuing education to maintain.
In 2020, that changed overnight: Every state issued a waiver and/or developed expedited telehealth licenses, allowing residents to meet virtually with doctors. By April 2020, over a third of all doctors’ appointments in the country were conducted via telehealth. Telehealth allowed contagious COVID patients to receive care without leaving their home. It also meant that for the first time, state borders weren’t a barrier for patients seeking life-saving care from faraway specialists.
“Telemedicine has improved health-care access,” a Washington Post columnist declared in 2022. “Let’s keep it.”
But state legislators and medical boards didn’t keep it: In state after state, starting as early as 2021, legislators and medical boards began rolling back telehealth access, ending waivers and—in most states—reverting to pre-pandemic restrictions.
30 states now have telehealth bans
As of December 2023, all waivers are gone. At least 30 states now either ban or severely restrict telehealth appointments with doctors licensed out-of-state.
If you live in the following states, you cannot have telehealth appointments with doctors licensed out-of-state:
Alabama, Alaska, Arkansas, California, Colorado, Connecticut, Hawaii, Idaho, Illinois, Iowa, Kentucky, Massachusetts, Michigan, Mississippi, Missouri, Montana, Nebraska, New Hampshire, New Jersey, New York, North Carolina, North Dakota, Ohio, Oklahoma, Rhode Island, South Carolina, South Dakota, Washington, Wisconsin, and Wyoming
There are limited exceptions in some of these states: In Alaska, for example, you can use telehealth to see an out-of-state doctor if you have a life-threatening condition, a referral from an Alaska-licensed physician, and a pre-existing relationship with the out-of-state doctor. In Iowa, audio-only calls aren’t classified as telehealth; only video calls are prohibited. In several states, out-of-state doctors can have telehealth consultations with doctors licensed in-state, but not calls with patients.
Kentucky, believe it or not, has a special carve-out for visiting sports teams. If you’re a doctor employed by a “sports entity visiting Kentucky for a specific sporting event,” you are allowed to treat the members, coaches, and staff of that team without a Kentucky medical license, via telemedicine or in-person. Similarly, federal legislation passed in 2018 ensures that sports medicine doctors who work for a team, athlete, or sports governing body can treat athletes across state lines.
It makes you wonder: If athletes are allowed to be treated by their preferred doctor even if the doctor isn’t licensed in that state, shouldn’t people who can’t score a touchdown also get that privilege?
In some states, including New Jersey, doctors can face criminal charges and even jail-time for practicing telemedicine with an out-of-state license. New Jersey’s telehealth restrictions are being challenged in a new lawsuit filed by Pacific Legal Foundation on behalf of Boston oncologist Shannon MacDonald, whose patients include a 13-year-old boy in New Jersey in remission from a rare cancer he battled for years. For that boy, and families like his in the 30 states that restrict telehealth, staying healthy relies on access to out-of-state specialists—access that state legislators have decided to cut off.
20 states have more permissive laws
The other 20 states (and the District of Columbia) have a wide range of regulatory processes and stipulations that make telehealth at least a little easier for patients.
The following eight states have created a special telehealth license that’s easier for out-of-state doctors to obtain than a full medical license in the state:
Georgia, Louisiana, Nevada, New Mexico, Oregon, Tennessee, Texas, and Vermont
Another eight states have made it even easier: Doctors only need to register with, or receive a waiver from, the state medical board to practice telehealth in the following eight states:
Arizona, Delaware, Florida, Indiana, Kansas, Maine, Minnesota, and West Virginia
Other states have reciprocity agreements. Doctors in the following regions are allowed to practice telehealth throughout the region, as long as they’re licensed by one of the three medical boards:
The District of Columbia, Maryland, and Virginia
Similarly, one state allows doctors from adjoining states to obtain a special telehealth license, as long as those states do the same:
Pennsylvania
Finally, one state freely allows doctors licensed out-of-state to practice telehealth if they’re doing it pro bono:
Utah
The future of telehealth
For doctors across the country—especially specialists with highly sought-after expertise—the current legal landscape for telehealth is a nightmare.
Kaytie Ravega, a healthcare attorney at Quarles & Brady, told “A Virtual View: A Telehealth Podcast” that doctors are struggling to understand “what they can do, where they can do it, and how to stay on top of that.”
Obtaining medical licenses in every single state simply isn’t a feasible option for doctors: The upfront fees and costs would exceed $90,000 and the annual renewal fees would top $11,000.
The only providers who can manage to conduct telehealth across the country are national giants: Amazon recently launched Amazon Clinic, which offers video telehealth calls in all 50 states. How? Because Amazon matches patients with a clinician licensed in their state, according to the FAQ.
That’s fine if you’re looking to treat eczema, pink eye, or high blood pressure—all common conditions listed on Amazon Clinic’s homepage—but what if you’re that 13-year-old boy in New Jersey, in remission from a rare cancer, whose life could be saved by regular telehealth calls with a Boston specialist?
In that case, your best hope for the future of telehealth may be PLF’s lawsuit, which, if successful, may start a movement to bring back telehealth everywhere.